How to make community surveillance more effective?
#13 - Our health workers are doing massive community surveillance; how can we make it more effective?
Our strategy for District Magistrates in India: COVID-19 is a war only Districts can fight.
Until tests are made available, community surveillance is the only way forward.
What can you do?
A war effort is necessary to screen each and every household in your district. The soldiers in this battle - ASHA workers need to be ready with the right knowledge and equipment.
ASHA workers, teachers and volunteers have done such community surveillance exercises in Goa and Rajasthan. However, one time surveillance does not help! Individuals have to be screened periodically to ensure that asymptomatic cases are not missed out.
For an individual in green districts we recommend screening every week, and every three days for yellow and red districts.
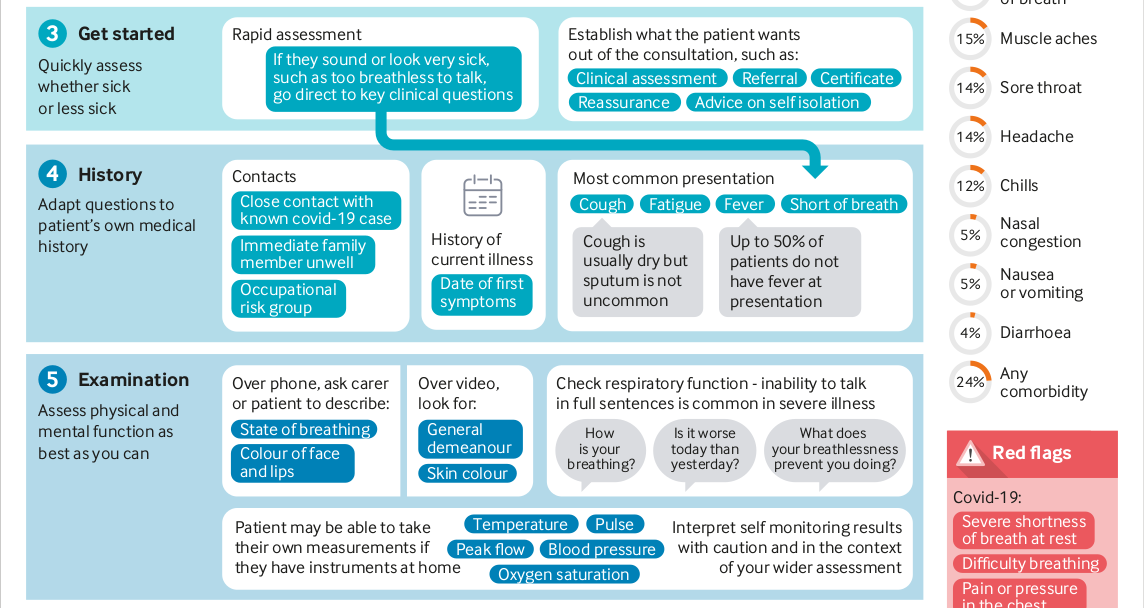
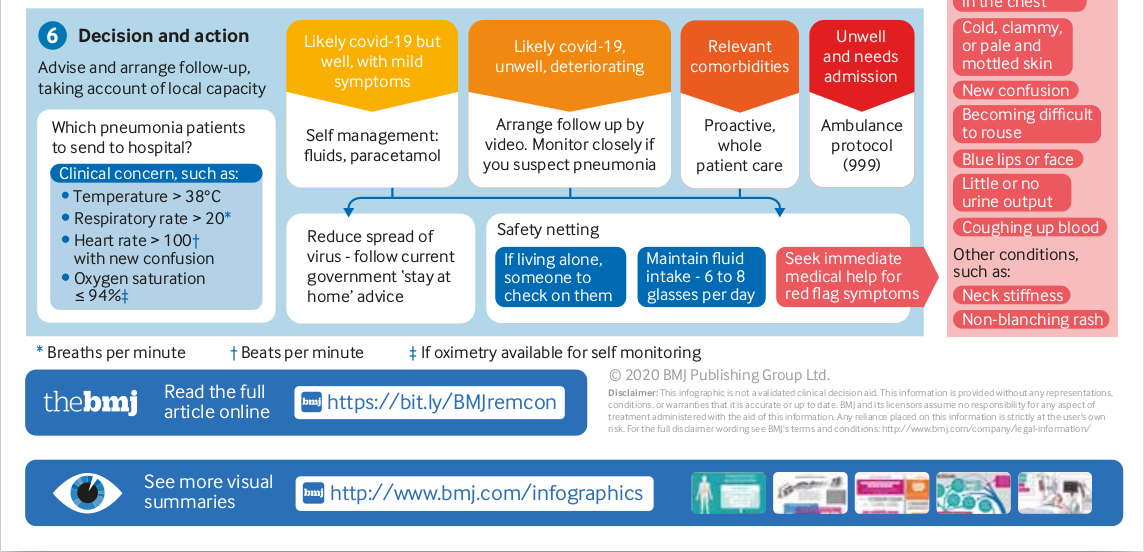
We outline two check lists for remote screening and door to door surveillance below :
1. A check list for community screening :
Up to three methods are given for the key symptoms that need to be kept track of, how to check them and quantify them are given. As a DM please decide on one of the options for effective monitoring of each symptom; enable your health workers with one of the options and record books so that we can more objectively assess the symptoms.
Temperature -> Objective measurement of the temperature is required -> Options ->
IR thermometer for each health worker. This will cost 4500-6000 per health worker, but is the best solution for objective measurement and recording of every individual.
Thermometers can be distributed to each household. Digital thermometers can be given; one each household. The visiting health worker can then ask each individual to check their temperature and make a record. The thermometer should be wiped between individuals. This will cost approximately 200-300 per household in the district and can also be seen as a philanthropic initiative.
Digital thermometers can be given to health workers along with thermometer probe covers. Health workers need to change the probe covers before checking every individual. The probe cover should be discarded in the household where it was used. The thermometer can be wiped with alcohol wipes between households.
Shortness of Breath -> Objective measurement of respiratory rate is required -> Options ->
Pulse oximetry. Each health worker can be provided a pulse oximeter. The health worker needs to note down respiratory rate and SpO2. Pulse oximeter should be wiped with alcohol between use. The individual should be given hand sanitiser before and after use of the pulse oximeter. The solution will cost 3000-4000/ health worker.
Manual breath count by a family member. The health worker needs to ask family members to count the pulse for other members for 30 seconds. This count can be recorded for each individual. Health workers shouldn't do it themselves to avoid risk of infection. Each individual should use hand sanitizer before and after the counting is done.
Roth score index is measured by having the patient count from 1 to 30 in their native language, in a single breath, as rapidly as possible. The primary result of the Roth score is the duration of time and the highest number reached. While this is not widely recommended to understand breathlessness; this technique can give a good measure of respiratory rate if the family members are not able to do a manual count.
Anosmia -> Objective measurement of loss of sense of smell is required
Ask every individual to identify 5 common household smells with their eyes closed. Do this for each individual in the family.
Physiological signs -> Subjective assessment by the health worker to identify severity -> Options ->
The health worker should note assessment of
a) wheezing, grunting or whistling sounds during breath
b) blueness of lips or in nails
c) nasal flaring or pursed lip breathingAudio recording of consultations: The health worker if provided with a smartphone or a recorder can record breath sound after asking every individual to take deep breaths. These can be analysed over a tele consulting platform.
Video recording conversations: The health worker; if provided with a smartphone can do video recording of their interaction with every individual. these recordings can then be assessed over a tele consulting platform.
2. A checklist for remote screening in urban centers :
If resources are available, a safer and contact less screening plan can be adopted.