Checklist for Effective Contact Tracing
#9 - Contact tracing is the key to isolate potential vectors and contain the outbreak. We cover basic guidelines and tools to ease this process.
Contact tracing is hard. But it remains the most efficient way of curbing the spread of infection.
Contact tracing involves finding and informing people that they have been in contact with another infected person so that the primary and secondary contacts can seek medical care. Contacts of the suspected/confirmed case of COVID-19 should then be isolated (if sick) or quarantined (if well) to lessen the spread of the virus.
Identified a COVID-19 suspect?
Do share the following checklist with all hospitals and responders under your jurisdiction.
5 steps to successful contact tracing
1: Understand how the virus spreads.
The COVID-19 virus is located in the respiratory tract and is spread when someone coughs or sneezes, dispersing infected droplets in the air. One sneeze or cough can spread infected droplets everywhere, even onto surfaces that people may touch later and hence several people can get infected from just one COVID-19 positive patient.
Contact tracing under these circumstances is challenging. The identified case will have to recall their movements carefully to identify all close contacts.
2: Ask the right questions
During contact tracing, remember that under 50% of infected individuals will show no symptoms. These individuals can still be infectious. Take steps to minimize damage.
Close contacts are those who have had face-to-face contact with a confirmed case for a period more than 15 minutes, or those who have shared an enclosed space with a confirmed case for more than two hours.
The contact tracer will be especially interested to know:
Who has this confirmed case met or talked with recently? Was it indoors or outdoors?
Who all were in close proximity? This is important in closed space settings such as restaurants/cafes, meetings, marketplaces, vehicles, mess/canteens..
Have they been to a big event like a religious gathering or celebration?
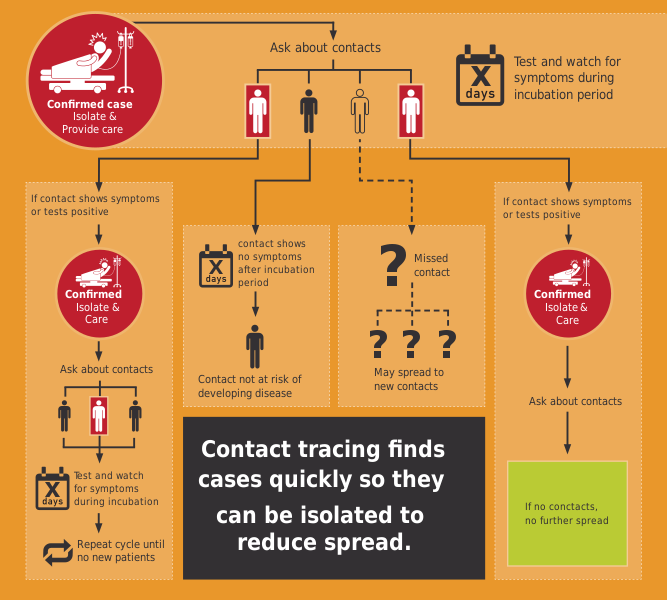
There are careful steps that we must take depending on who our primary (index) case is. The checklist linked above can help as a tool during investigations.
By CFCF - Own work, CC BY-SA 4.0, Wikimedia
3: Use the right technological tools
AarogyaSetu an app launched and endorsed by the Government of India can be an effective tool in contact tracing in more crowded urban centers. AarogyaSetu sends a notification in case an individual has come in contact with another person who might be positive and also shows the risk of infection. The requirement of an internet-enabled smartphone may act as a limitation.
Some text-based tools such as Whispir can be used for bulk messaging and forwards which can then be triaged for identifying contacts. Such tools for the Indian context are still under development.
4: Enable active monitoring & ensure quarantine compliance
Once the contacts of the primary patient have been identified, it is essential that they are
Actively monitored
Provided proper guidance on home isolation and quarantine
Provided medical care as soon as symptoms progress.
5: Dispel the stigma around COVID-19
Being sick is not a crime. We need to appropriately counsel first and second-order contacts to encourage them to seek medical attention and also disclose names of those who they may have come in contact with. The option of medical anonymity should be provided to the suspected individuals so that they are encouraged to seek medical attention.
Our strategy for District Magistrates in India: COVID-19 is a war only Districts can fight.
We wish to help you end the outbreak.
Get the best tactics, tech, and support.
We write from the India chapter of endcoronavirus.org! Our efforts were critical in the US in banning flights from China in Jan & other early outbreak control measures in India & the EU.
We’re assisting Indian administrators in understanding and acting on the COVID-19 situation. Join 4 other states, 13 districts who are working with us!

